Can a holistic diet help patients with esophageal cancer?
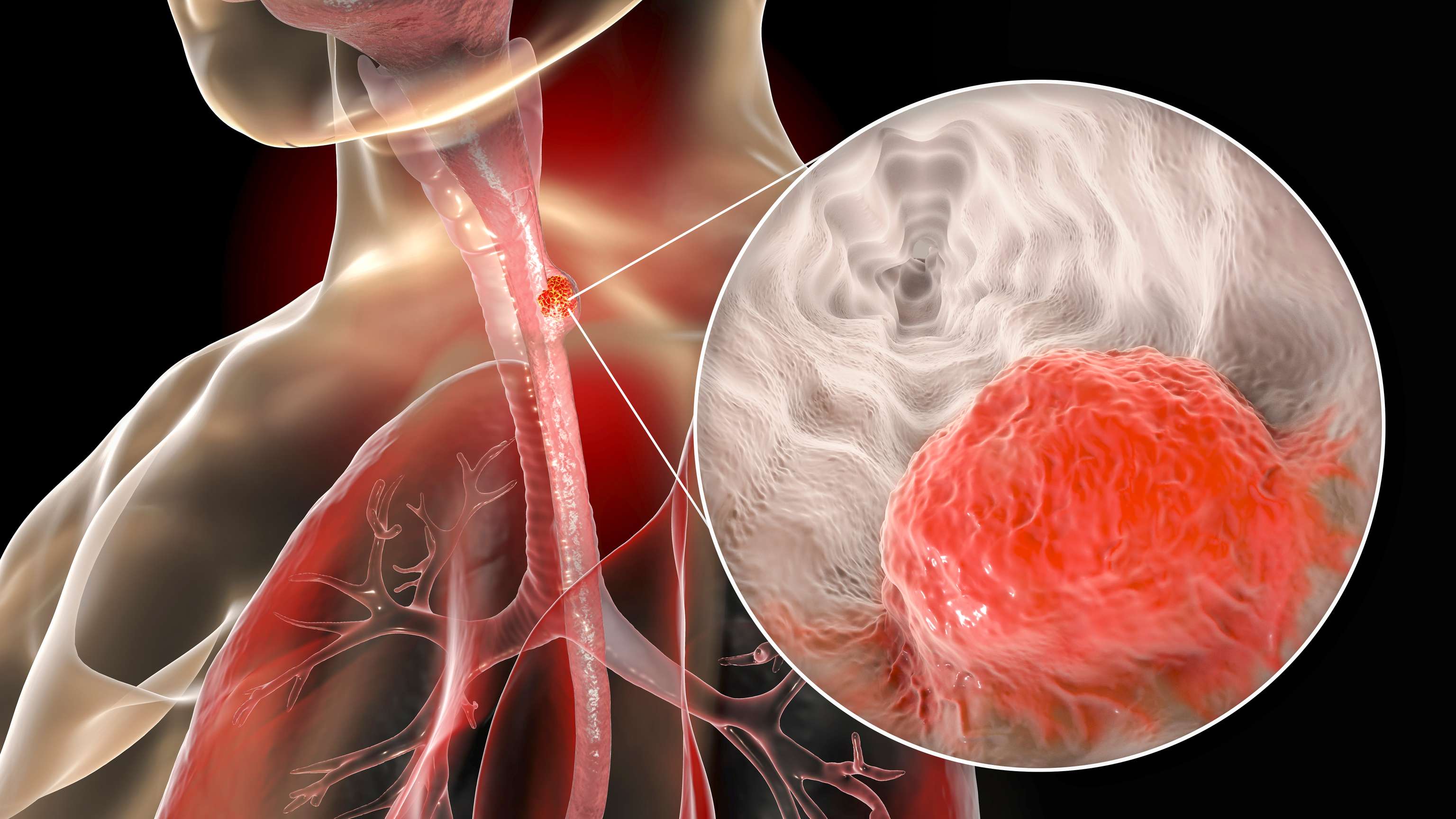
Esophageal cancer:
Esophageal cancer, also known technically as esophagealcancer, is a cancer of the esophagus and the junction of the esophagus and stomach. Globally, in 2012, about more than 80% of deaths identified with esophageal cancer were reported in developing countries, especially in mainland China.
In this regard, it is believed that unfavorable lifestyle, characterized by excessive alcohol and nicotine consumption, as well as overeating, could be a possible factor for the increasing cases of the disease in Western countries. This could also promote reflux disease (i.e. gastric juice enters the esophagus and damages the mucosa), which is involved in the development of adenocarcinoma (i.e. subtype of esophageal cancer).
In this context, malnutrition often leads to complications in patients with esophageal cancer. Researchers from the study, published in 2020, believe that a holistic dietary approach could help minimize such adverse effects.
Between 40% to 80% of all cancer patients suffer from malnutrition, which is highest in patients with esophageal cancer at 67-80%. Radiochemotherapy (i.e., combination of radiation therapy and chemotherapy) has become the most significant means of treating this carcinoma, according to researchers. At the same time, malnutrition can possess many negative effects, such as increased treatment toxicity, prolonged hospital stay, and short-term increased readmission rate.
Henan study:
Because little evidence exists regarding the effect of diet on patients with esophageal cancer, the research subjects investigated the efficacy of a holistic diet on the prognosis or complications of radiochemotherapy as part of a controlled trial. For this purpose, the randomized trial published in 2020, in the journal Nutrition, analyzed 96 patients with esophageal cancer (with radiochemotherapy) in Henan Cancer Hospital, Zhengzhou University, from April 2017 to March 2018.
Study participants were numbered in order of hospital admission and randomly divided into two groups with written informed consent. Among them, the inclusion criteria were as follows:
- At least 18 years of age
- Indications for concurrent radiochemotherapy were met
- No serious cardiovascular or cerebrovascular disease (i.e., atherosclerotic change in the arterial vessels of the brain)
Study participants had to be conscious, show no problems with communication, walk without external assistance, and sign an informed consent form.
Exclusion criteria included:
- Organ transplantation
- Simultaneous occurrence of other malignant diseases, liver or kidney dysfunction
- Endocrine disorders, metabolic disorders, or other digestive tract disorders.
While the intervention group was treated with a holistic nutritional approach by a "Nutrition Support Team" in a time window of 6 weeks, study participants of the control group received a general nutritional approach during this period. The nutritional model for the intervention group was developed jointly by a dietitian and an oncologist. The control group received a general dietary supplement of protein, fat, carbohydrates, fiber, minerals, and essential vitamins.
From the beginning of the study, the subjectively perceived overall score was analyzed every week before discharge, as well as the blood index, quality of life and psychological state of the patients.
Potential complications such as radiation esophagitis (i.e., esophageal inflammation), completion rate of therapy and clinical outcomes were measured by the researchers.
Significant study outcomes:
Of the 96 study participants, 45 in the intervention group and 40 in the control group completed it. Significant differences in serum albumin and total protein changes were seen throughout the study period. The serum albumin shows the concentration of the plasma protein albuminin the blood serum, which can show a possible lack of protein in the liver area or highlight a loss of protein affecting the kidney. Also the Analyzed complications and quality of life were significantly different before and after the study phase.
Conclusion:
The study results of the analysis suggest that a holistic dietary plan designed by dietitians and oncologists during the phase of radiochemotherapy, could maintain or even improve the nutritional status of patients with esophageal cancer. Thereby, the severity of radiation esophagitis was minimized, quality of life and depressive symptoms were improved. More larger randomized longitudinal controlled clinical trials are needed to accurately analyze the dynamic changes in these indicators and to better understand the importance of nutrition in patients with such type of carcinoma and radiochemotherapy.
Sources
- Qiu Y, You J, Wang K, Cao Y, Hu Y, Zhang H, Fu R, Sun Y, Chen H, Yuan L, Lyu Q. Effect of whole-course nutrition management on patients with esophageal cancer undergoing concurrent chemoradiotherapy: A randomized control trial. Nutrition. 2020 Jan;69:110558. doi: 10.1016/j.nut.2019.110558. Epub 2019 Jul 23.
- Speiseröhrenkrebs (NetDoktor)
- Information der deutschen Krebsgesellschaft

Danilo Glisic
Last updated on 12.05.2022
Your personal medication assistant
Browse our extensive database of medications from A-Z, including effects, side effects, and dosage.
All active ingredients with their effects, applications, and side effects, as well as the medications they are contained in.
Symptoms, causes, and treatments for common diseases and injuries.
The presented content does not replace the original package insert of the medication, especially regarding the dosage and effects of individual products. We cannot assume liability for the accuracy of the data, as the data has been partially converted automatically. Always consult a doctor for diagnoses and other health-related questions.
© medikamio