Monkeypox in Europe: current situation, distribution and vaccination.
Disease pattern, transmission, therapy - all important information.
This type of smallpox is a viral disease that can be transmitted from animals to humans as well as from humans to humans. This type of smallpox is triggered by the virus genus Orthopoxvirus simiae, which is also involved in the classic smallpox viruses (variola). In Africa, the viruses are mainly found among rodents, not in monkeys. The virus is named "monkeypox" because it was first observed in monkeys in the laboratory (1958). In humans, the virus was first discovered in Congo in 1970. Infected was a baby at 9 months of age and since then other cases of this infectious disease in humans have been reported. These occur primarily in West and Central Africa. Monkeypox in humans was not reported outside Africa until 2003, and to date only isolated cases of the viral disease have been reported outside Africa. Presumably, the virus was brought out of the country by importing animals from Africa. Currently, the infection occurs exclusively through human-to-human infection.
In humans, the disease is usually mild and self-healing. Exceptions are people with a weak immune system and children. The symptoms have so far been much milder than smallpox (variola), which was declared eradicated in 1980. The most common symptoms include fever, chills, headache, muscle aches and fatigue. Characteristic, however, are skin lesions (rashes) that first appear patchy and progress to pustules until they dry, crust over, and fall off. The rashes can appear on the face, as well as in the genital area, on the hands and feet, and on the chest. The pustules may also appear on mucous membranes. As a rule, the rash is completely healed after four weeks at the latest.
Monkeypox viruses are transmitted through close physical contact, contact with bodily fluids or via the rashes typical of the disease. Transmission via droplet infection cannot be ruled out either. Affected persons are contagious until the rashes have completely healed. Transmission can also occur via objects (e.g. towels, bed linen, door handles) that an infected person has touched/used. In affected areas in Africa, transmission can also occur from animals to humans, usually then from rodents. Animals transmit the viral infection via bites, extremities, secretions, and contaminated fur or material. The incubation period lasts at least 3 to a maximum of 21 days.
Skin and body contact with infected individuals should be limited and open wounds or rashes should not be touched. Sexual contact should also be prevented for the time being, as infection can also be transmitted via sexual intercourse. Condoms can reduce the risk of infection, but cannot prevent it. Incidentally, the use of condoms is still strongly recommended up to eight weeks after the rashes have healed. The virus has been shown to persist in seminal fluid for some time.
Anyone infected with monkeypox must go into quarantine for at least 21 days from the first day symptoms appear. If infection is asymptomatic and diagnosed via specimen collection, isolation begins from the time the specimen is collected. Quarantine may be lifted when rashes are completely healed. Samples are collected from weeping wounds, vesicles, pustules, and crusts. Swabs from skin lesions are also a common method of diagnosis. Although monkeypox belongs to the same genus as human smallpox, which was declared eradicated in 1980, symptoms are milder and the risk of death is much lower. Only patients with typical symptoms and risk factors (travel to endemic areas) are usually tested for infection with these smallpox viruses. Anyone who notices symptoms themselves is best to go into quarantine immediately and seek advice from the health department or family doctor.
Treatment is usually uncomplicated, as the infection clears up on its own within a few weeks (severe courses are possible, however). Therapy is only supportive, so that superinfections via bacteria do not occur. Only recently, the drug Tecovirimat was approved in the EU for the treatment of the viral infection and is also available in Germany to a limited extent.
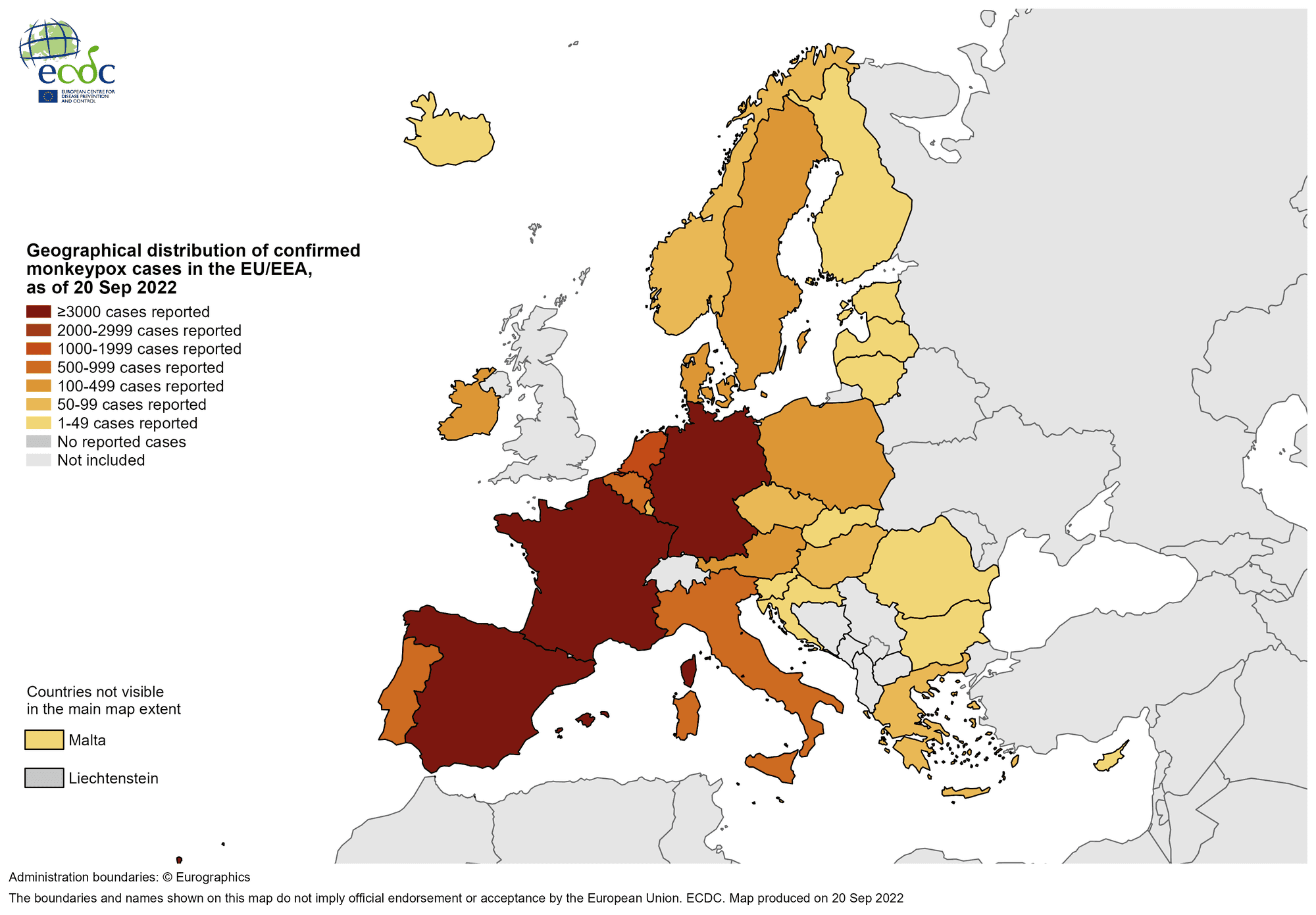
Current situation and development in Europe
According to the Global Health Network, more than 64,000 monkeypox cases have currently been confirmed worldwide between January and September 2022. Already 3,570 cases of these come from Germany. Registered are such cases outside the African continent since the spring of 2022, in which the affected persons did not come from endemic countries. What has become known in this country is primarily the assumed transmission of the virus via sexual intercourse.
The Robert Koch Institute and the World Health Organization are monitoring and analyzing the current cases and constantly updating the status of their research and findings. In order to assess the risk for Europe and Germany, the development of transmission and research must be accurately recorded. In July 2022, the World Health Organization (WHO) declared the viral disease a "health emergency of international concern." Recommendations include isolation or quarantine and proper treatment of those infected, as well as contact tracing, vaccination and better communication to contain the virus. So far, the general German population does not experience any health risk, as this type of smallpox is only contagious in this country under certain conditions. The same applies to the whole of Europe. So far, monkeypox has not been able to establish itself as a pandemic infectious disease in Europe. Nevertheless, it is listed worldwide as an epidemic that is usually transmitted from person to person. If no preventive measures are taken, there is a real risk that the infections will reach pandemic proportions worldwide. The current outbreak in Europe should be further limited by taking precautions and detecting infections promptly.
In principle, the knowledge and experience gained from the Covid pandemic can also be used in epidemics such as this infectious disease. Early detection, quarantine measures, reporting of illnesses, and education campaigns can help to continue to protect the population and prevent another pandemic.
All about monkeypox vaccination
(Human) smallpox was declared eradicated in 1980 and vaccination was discontinued. Until then, smallpox vaccination was even mandatory. Since 2013, a new smallpox vaccine (Imvanex) has been available in the EU, which can also be used for monkeypox cases. However, only people 18 years of age and older may be vaccinated. The Robert Koch Institute and the Standing Commission on Vaccination (STIKO) provide comprehensive information on vaccination options and new developments. Currently, only certain risk groups should consider vaccination, for example immunocompromised people. Otherwise, vaccination is not currently recommended and is not yet considered mandatory.
According to the STIKO, vaccination should be carried out with the vaccine Imvanex/Jynneos/Imvamune. The basic immunization consists of two vaccination doses. The second dose is given after at least 28 days. The first dose guarantees a good basic protection after only 14 days, the second dose prolongs the vaccination protection. If one has already received the smallpox vaccination in the past, a single dose of vaccination is sufficient. Two booster vaccinations are recommended for immunocompromised people who have already been vaccinated against smallpox.
Vaccination against smallpox is administered through the skin, i.e. subcutaneously. Anyone who has been in contact with an infected person can be vaccinated preventively, but within 14 days of contact and as long as there are no symptoms. If the vaccination is given immediately after contact, the infection can be prevented. If the vaccination is given only after four to a maximum of 14 days, the infection cannot be prevented, but symptoms can be alleviated. Whether the Imvanex vaccine is effective in children has not yet been adequately researched. Because the vaccine is in limited supply, doses are distributed to the states and provinces.
Will the disease continue to be a problem in the future?
Throughout Europe and in this country, the development of the spread of monkeypox is constantly monitored. New findings and information are regularly available, and health offices are also happy to provide information. Above all, preventive measures are important, giving more time to current research. Infected persons should be treated and postexposure measures should be taken. In addition, it is becoming increasingly important to educate and inform the population. Resources for prevention, such as testing and more vaccine doses for countries, should be increased.
Sources
- Goyal L, Ajmera K, Pandit R, Pandit T. Prevention and Treatment of Monkeypox: A Step-by-Step Guide for Healthcare Professionals and General Population. Cureus. 2022 Aug 21;14(8):e28230. doi: 10.7759/cureus.28230. PMID: 36017480; PMCID: PMC9393027.
- Chatterjee S, Sharma AR, Bhattacharya M, Dhama K, Lee SS, Chakraborty C. Relooking the monkeypox virus during this present outbreak: epidemiology to therapeutics and vaccines. Eur Rev Med Pharmacol Sci. 2022 Aug;26(16):5991-6003. doi: 10.26355/eurrev_202208_29541. PMID: 36066177.
- Internationaler Affenpocken-Ausbruch: Fallzahlen und Einschätzung der Situation in Deutschland (Robert Koch Institut)
- Antworten auf häufig gestellte Fragen zu Affenpocken (Robert Koch Institut)
- Schutzimpfung gegen Affenpocken: Häufig gestellte Fragen und Antworten (Robert Koch Institut)
- Global.health Monkeypox Map
Medikamio
Last updated on 27.09.2022
Your personal medication assistant
Browse our extensive database of medications from A-Z, including effects, side effects, and dosage.
All active ingredients with their effects, applications, and side effects, as well as the medications they are contained in.
Symptoms, causes, and treatments for common diseases and injuries.
The presented content does not replace the original package insert of the medication, especially regarding the dosage and effects of individual products. We cannot assume liability for the accuracy of the data, as the data has been partially converted automatically. Always consult a doctor for diagnoses and other health-related questions.
© medikamio